REPORT
Clinical Study Report
“Application of the Tonometer for Intraocular Pressure Measurements: EASYTON in Patients in the Early Postoperative Recovery Phase following Penetrating Keratoplasty”
Rationale
Penetrating keratoplasty is a surgical transplantation procedure used for treatment of a variety of severe corneal diseases. In some cases, the postoperative period is complicated by increased intraocular pressure, which worsens prognosis and requires correction of the treatment plan. Measurement of intraocular pressure bears the risk of injuring the graft and significantly changing the biomechanics of the cornea, which in turn prevents accurate measurement. For this reason, it is not uncommon for specialists to rely on finger palpation to determine IOP during the postoperative period. Palpation also allows the measurement to be taken through the eyelid in the area where the sclera is intact, thus not affecting the corneal graft.
This circumstance is particularly suited to clinical use of an advanced transpalpebral tonometry technique that doesn’t affect the cornea and provides reproducible results with high accuracy and objectivity.
Research title
“Application of Tonometer for Intraocular Pressure Measurements: Use of EASYTON in Patients following Penetrating Keratoplasty”
Design of the study:
This was conducted as an observational clinical controlled study.
Clinical base for the scientific and clinical research
State Budgetary Healthcare Institution “Samara Regional Clinical Ophthalmology Hospital named after T.I.Eroshevsky”, operating under license for medical activity No. ЛО-63-01-004259 dd. 31.05.2017
Chief Researcher (full name, job title)
Elena Vladimirovna Karlova, Doctor of Medicine, Board Certified Ophthalmologist, Head of the Glaucoma Microsurgery Department.
Duration of Study
7 weeks
Purpose
To study the effectiveness (accuracy of measurement of intraocular pressure) and safety in use of the EASYTON Tonometer for determination of intraocular pressure in patients during the early postoperative recovery phase following penetrating keratoplasty.
Objectives
- Daily comparative measurements of IOP in participants (subjects) using both the palpation method and EASYTON tonometer transpalpebral method during the first seven days following penetrating keratoplasty.
- Comparative analysis of the accuracy of IOP values obtained with the palpation method and with EASYTON.
- Registration (if any) of all adverse events that occurred while operating the tonometer during the study period, followed by an assessment of the safety of the tonometer.
Material and methods of research
The study subjects comprised 43 patients in the early recovery phase after penetrating keratoplasty. The intraocular pressure (hereinafter “IOP”) was measured with the EASYTON tonometer for IOP measurements (hereinafter “the tonometer”).
The initial selection was performed by the principal researcher based on the analysis of initial medical documentation on the subjects of research undergoing treatment and examination at the State Budgetary Healthcare Institution “Samara Regional Clinical Ophthalmology Hospital named after T.I.Eroshevsky”, as well as based on the inclusion and exclusion criteria of this study. The length of the study for each patient was 7 calendar days.
Characteristics of Subjects
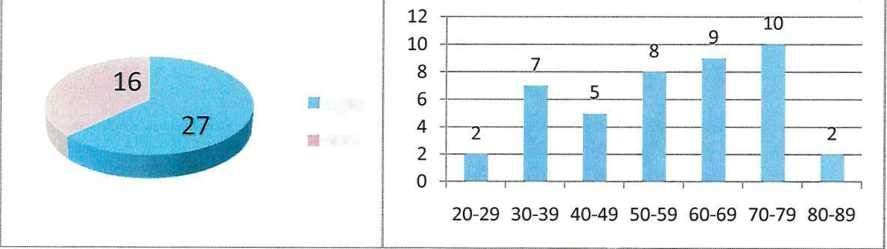
- Gender: 27 Male, 16 female – see Figure 1;
- Age: from 28 to 86 years (distribution is shown in Figure 2);
- Social status: 11 in employment, 3 unemployed, disabled; 29 unemployed, pensioners.
Absence of exclusion criteria
Exclusion criteria
- pathology of the upper eyelid (inflammatory diseases, scars, deformation of the eyelid);
- evident pathology of the sclera in the area of measurement.
The EASYTON tonometer is designed to measure intraocular pressure through the eyelid without the use of anaesthetics.
Contraindications to the use of EASYTON tonometer:
- pathological conditions of the upper eyelid (inflammatory diseases, scars, deformation of the eyelid)
- evident pathology of the sclera in the area of measurement.
The tonometer has two modes for IOP measurement:
- Maklakov scale IOP measurement mode
- Goldman scale IOP measurement mode
IOP measurement is performed through the eyelid. This eliminates contact with the sclera and cornea and does not require anaesthetics.
The operating principle of the tonometer is based on measuring intraocular pressure by registering the frequency of forced vibrations of eye tissues effected by the tonometer vibrator.
During the measurement, the rod is placed upon the eyelid in the scleral area and compresses it with a weight of about 10 g. This creates a single coupled “rod-eye” biomechanical system, the frequency of vibrations of which is considered to be the actual intraocular pressure.
The excitation of the vibrations is generated with the help of short electromagnetic pulses acting on the vibrator rod. The movement of the rod is transferred to the eye through the eyelid in the form of a short-term pulse that excites forced vibrations of the eye tissues.
The conversion of mechanical vibrations of the eye tissues into an electrical signal is performed by the tonometer’s electromagnetic system, which is structurally connected to the rod.
The oscillation period is measured by the tonometer and is used to calculate the IOP, which is displayed on the tonometer display.
The operating procedure of the tonometer
To ensure the accuracy of IOP measurement taken with the EASYTON tonometer for intraocular pressure measurements, the subjects were placed in a sitting position. The alignment of the head was as close to horizontal as possible. At the same time, the eyes were focused on the test object and the line of sight was at an angle of 45°. For correct fixation of the line of sight the test object was represented by a thumb raised up at an angle of 45° to the plane of the face.
In each patient, IOP was measured daily for seven days after the surgery by an experienced Glaucoma Department Employee using the palpation method, and then with the EASYTON tonometer. IOP measurement was performed in the following order:
- measurement of IOP of the eye which underwent surgery with EASYTON tonometer (three measurements);
- measurement of IOP of the eye which underwent surgery using the palpation method.
The results of IOP measurements were recorded in the individual registration cards of the subjects of the clinical study. A total of 301 IOP measurements with the EASYTON tonometer were registered within the 7 days (in case of the three measurement series the average of these values was registered as the result).
Statistical processing of the obtained data included calculation of the average value and standard deviation (M±SD) and the Student’s t-test. The significance of differences was considered as statistically reliable at the level of p<0.05.
Results
Table 1 shows the average values of intraocular pressure measured in all 43 patients (43 eyes) who underwent penetrating keratoplasty and the average value of all measurements taken within the 7 measurement days. The measurements were taken using both methods on each measurement day.
Table 1
| IOP measurement method | Day of measurement (postoperative period) | Average Measure-ment over the 7 days | ||||||
| I | II | III | IV | V | VI | VII | ||
| Palpation | 14.95±5. 26 | 15.70±4. 72 | 15.88±5. 10 | 15.79±4. 41 | 16.49±4. 33 | 15.72±4. 48 | 16.09±4. 52 | 15.80±4. 68 |
| EASYTON | 15.24±4. 31 | 15.93±4. 94 | 16.19±4. 58 | 16.05±3. 85 | 17.14±4. 28 | 16.81±4. 29 | 16.70±4. 22 | 16.28±4. 36 |
The comparative analysis of the obtained data showed that the IOP of the same eyes of the same subjects were significantly statistically different (p=0.003714).
At the same time, the average IOP values determined using EASYTON tonometer were generally higher than those with the palpation method, which indicates a downward bias of the IOP values measured with palpation. The spread of the values of the three IOP measurements (average value of the three measurement series) was 1 mm Hg in 66.6% of the cases, and 2 mm Hg in 33.3% of the cases, indicating a high level of verifiability of IOP measurements taken with EASYTON tonometer.
The comparability of the measurements taken with EASYTON and with the palpation method was analyzed using the Bland–Altman plot.
Figure 3: Comparability of IOP measurements
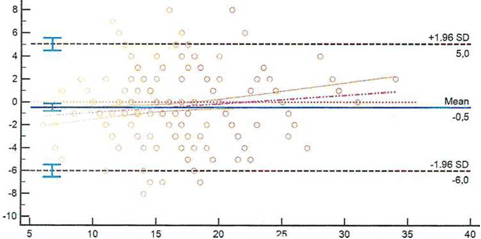
Based on the analysis of the entire patient group, we concluded that measurement results obtained using the EASYTON tonometer are not comparable to the measurements obtained by palpation.
The monitoring of occurrences of adverse events, as performed in the course of the current study, did not reveal any adverse effects related either to the use of EASYTON or the palpation method in any of the study participants.
No difficulties in the operation of EASYTON tonometer or design flaws were identified.
Conclusions
The study demonstrated the feasibility of using EASYTON for measurement of intraocular pressure in patients during the postoperative period after penetrating keratoplasty. This method is a safe and more accurate alternative to the currently used palpation method. The absence of corneal damage or adverse events during the study as well as the accuracy of the results determine EASYTON’s suitability for this category of patients. In addition, analysis of the IOP measurements taken within the three-measurement series showed a high level of reproducibility of results in each patient.
